We’re Changing the Cardiology Experience
Because You Deserve Better Care.
The practice of medicine, especially preventive cardiology, is failing patients because it focuses on general guidelines based mostly on numbers: “What’s your LDL?”, “What’s your BMI?” And that’s usually where it stops. It’s dangerous because it focuses on an equation instead of the individual. You are not your numbers. Your body is unique and deserves to be treated as such. We need a transformative shift in cardiology and preventive health care that considers you as an individual.
Let’s Talk
Send us a message and let us know how we can help you.
Introducing
Concierge Preventive Cardiology
with Dr. Scher
What if you could combine…
Now with Dr. Scher’s Concierge Preventative Cardiology, you can!
WELCOME TO
BOUNDLESS HEALTH WITH DR. SCHER
a revolutionary approach to optimizing your health and life!
Find out if this works for you
Connect with Dr. Scher today to see if this model is right for you.
Let’s Talk
Send us a message and let us know how we can help you.
Meet Dr. Scher, MD
CREATOR OF CONCIERGE PREVENTIVE CARDIOLOGY

Hi, I’m Dr. Bret Scher, and I’m changing the direction of preventive cardiology to better you with the care you deserve. I’m also the CEO and Lead Physician at Boundless Health and the Low Carb Cardiologist. I spent the past 15 years as a frustrated cardiologist. My patients weren’t achieving their optimal health, and I didn’t have the time or resources to guide them. That’s why I am revolutionizing my practice of medicine, and why I sought out additional certifications in lipidology, nutrition, personal training, functional medicine, and behavioral change.
It is through this specialized training and working with thousands of patients I recognized how to provide better care. Your health is too important to trust to guidelines designed for the ‘average’ person. You are not average, nor should you want to be!
I also recognize the need for better access and convenience. That’s the heartbeat behind Concierge Preventive Cardiology: open access so together, we can evaluate every facet of who you are and how you can best achieve your goals.
I’m glad you’re here. It tells me you know you deserve better care. I can’t wait to get started finding your path to true health.
Bret Scher, MD FACC
Board Certified Cardiologist and Lipidologist
Yes, People LOVE Dr. Scher’s Approach

We hear the words Heart Healthy a lot, especially when it comes to our nutrition.
By now, you’re likely used to seeing cereals with the “heart healthy” moniker. Is it really heart healthy? We all too frequently refer to foods as “heart healthy”, or we say that our doctor gave our hearts a “healthy” checkup.
It all sounds nice. But what does it mean? How do we define heart health?
How does LDL Cholesterol affect Heart Health?
Unfortunately, most of our current definitions center around LDL cholesterol concentration. While LDL cholesterol plays a role in heart health, it by no means defines heart health in totality.
In fact, in many cases it is the least important factor.
Our healthcare system has simplified things too much, so as a result we focus on one bad guy, one demon to fight. In reality heart disease is caused, and made more likely to occur, by a constellation of contributing issues.
Elevated blood sugar, elevated insulin levels, inflammation, high blood pressure, poor nutrition, and yes, lipids all contribute to heart health. It does us all an injustice to over simplify it to one single cause.
What food is heart healthy?
Our superficial definition of cardiac risk is how industrial seed oils containing polyunsaturated fatty acids (PUFAs) became known as “heart healthy.”
Studies show that they can lower LDL. But they can also increase inflammation and have no clinical benefit and even increase risk of dying. According to our simplified definitions, that doesn’t stop them from being defined as “heart healthy.”
That’s right! Something that increases our risk of dying is still termed “heart healthy.” How’s that for a backwards medical system?!
Same for blood sugar. If you have a diagnosis of Type 2 Diabetes (DM2) that is a risk for cardiovascular disease. If you don’t have the diagnosis, you are fine. That ignores the disease of insulin resistance that can predate diabetes for decades and increases the risk of heart disease and possibly even cancer and dementia.
Cereal can also be called “heart healthy” as they may minimally lower LDL. But is that a good thing if they contain grains that also worsen your insulin resistance and metabolic syndrome? I say definitely not.
Time has come to stop this basic, simplified evaluation and start looking at the whole picture.
How Low Carb High Fat Diets Improve Heart Health
Low carb high fat diets have been vilified as they can increase LDL. But the fact of the matter is that it does so only in a minority of people. The truth is that they can improve everything else!
These diets reduce blood pressure, reduce inflammation, improve HDL and triglycerides, and reverse diabetes and metabolic syndrome! Shouldn’t that be the definition of “heart healthy” we seek? Instead of focusing on one isolated marker, shouldn’t we define heart health by looking at the whole patient?
Only by opening our eyes and seeing the whole picture of heart healthy lifestyles can we truly make an impact on our cardiovascular risk and achieve the health we deserve.
Join me in demanding more. Demand better.
Thanks for reading,
Bret Scher, MD FACC

Despite what the sugary beverage and processed snack food companies want us to believe, all calories are not created equal.
A new study from Harvard shows that individuals following a low-carbohydrate (20% of total calories) diet burn between 209 and 278 more calories per day than those on a high-carbohydrate (60% of total calories) diet. So the type of calories we eat really does matter.
The New York Times: How a low-carb diet might help you maintain a healthy weight
This isn’t the first study to investigate this topic, but it is likely the best.
The current study was a meticulously controlled, randomized trial, lasting 20 weeks. Even more impressive, the study group provided all the food for participants, over 100,000 meals and snacks costing $12 million for the entire study! This eliminated an important variable in nutrition studies — did the subjects actually comply with the diet — and shows the power of philanthropy and partnerships in supporting high-quality science.
After a run-in period where all subjects lost the same amount of weight, participants were randomized to one of three diets: 20% carbs, 40% carb, or 60% carbs, with the protein remaining fixed at 20%. Importantly, calories were adjusted to stabilize weight and halt further weight loss, thus making it much more likely that any observed difference in calorie expenditure was not from weight loss, but rather from the types of food consumed.
After five months, those on the low-carb diet increased their resting energy expenditure by over 200 calories per day, whereas the high-carb group initially decreased their resting energy expenditure, exposing a clear difference between the groups. In addition, those who had the highest baseline insulin levels saw an even more impressive 308-calorie increase on the low-carb diet, suggesting a subset that may benefit even more from carbohydrate restriction.
Why is this important? It shows why the conventional wisdom to eat less, move more and count your calories is not the best path to weight loss. Numerous studies show better weight loss with low-carb diets compared to low-fat diets, and now studies like this one help us understand why.
Our bodies are not simple calorimeters keeping track of how much we eat and how much we burn. Instead, we have intricate hormonal responses to the types of food we eat. It’s time to accept this and get rid of the outdated calories in-calories, calories-out model, thus allowing for more effective and sustainable long-term weight loss.
Originally Posted on the Diet Doctor Blog

What do I mean by “misunderstood?” Look no further than the common misnomer of “good” or “bad” cholesterol.
Good and Bad Cholesterol
While it may be true that High-Density Lipoprotein (HDL) has potentially beneficial functions (reverse cholesterol transport), we have to remember there is no such thing as good and bad cholesterol. The cholesterol carried by HDL is the same as that carried by LDL. The only thing that makes it good or bad is if it ends up synthesizing our hormones or bile acids (good), or if it ends up in our vessel walls (bad).
If it’s true there is no such thing as good and bad cholesterol, why do we care about our HDL levels?
First, let’s start with the basics.
HDL is the smallest and most densely packed lipoprotein and has one or more ApoA protein on its surface. HDL can help lipids move around in circulation by accepting triglycerides or cholesterol from other particles, thus helping a VLDL turn into an LDL, or helping an LDL contain less cholesterol (turning a small dense LDL into a less densely packed LDL).
Like LDL, HDL transports cholesterol to the liver for recycling or excretion, or to the hormone producing cells like in the adrenals. Unlike LDL, HDL does not have the potential to get retained in the vascular wall and does not, therefore, contribute to plaque formation. In fact, functioning HDL can remove cholesterol from the vessel wall, thus putting it back into circulation and possibly removing it from the body.
Back to the question at hand.
Why should we care about HDL levels?
Early epidemiological trials showed that lower HDL levels were associated with a higher risk of cardiovascular disease and even death. With such a strong association, the medical profession promoted elevated HDL levels as protective and low levels as something we need to avoid.
Since these were observational epidemiological studies, they do not prove that the low HDL caused the problems, only that HDL was associated with it. For instance, HDL is also known to be low in diabetes, metabolic syndrome and insulin resistance. It may, therefore, simply be a marker of underlying metabolic dysfunction that contributes to increased risk. Yet, HDL’s function in reverse cholesterol transport, and its ability to remove cholesterol from vessel walls suggests a more direct impact on cardiovascular health.
It is also important to note that the Framingham data suggested that increased cardiovascular risk with elevated total cholesterol and LDL-C was lost in the presence of high HDL. In fact, very low levels of LDL combined with very low HDL levels had a much higher risk than markedly elevated LDL levels when combined with elevated HDL.
Thus, HDL proves to be a useful marker to help predict cardiovascular risk. For instance, one large meta-analysis showed that total cholesterol/HDL ratio was a much stronger predictor of cardiac mortality than total cholesterol alone.
In addition, the PURE study, an observational trial in over 135,000 subjects, showed that when considering lipid changes brought about by nutritional changes, ApoB/ApoA1 (essentially LDL-P/HDL-P ratio) is the best predictor of clinical outcomes.
Thus, HDL level is important in assessing cardiovascular risk.
Drugs Muddy the Picture
While HDL may be a good predictor of risk, raising it with drugs does not seem to confer added benefit.
For instance, cholesterol ester transferase protein inhibitors (CETP inhibitors) significantly reduced LDL by 20-30% and increased HDL 100-fold, yet showed either no clinical benefit or even worse, an increased risk of death.
This was a shock to many in the lipid world as the notion of “good” and “bad” cholesterol would clearly predict lowering LDL and raising HDL would confer dramatic health benefits. So much so, that multiple pharmaceutical companies invested hundreds of millions of dollars developing these drugs only to abandon them when the trials showed no benefit.
Part of the issue is that not all HDL lipoproteins function the same. There are subsets of people with genetically determined markedly elevated HDL levels who have an increased risk of CVD. They may have plenty of cholesterol circulating in HDL particles, but the HDL particles are dysfunctional and therefore do not effectively remove cholesterol from vessel walls or LDL and do not effectively transport it to the liver. Conversely, there are those with a specific genetic mutation called ApoA1 Milano who have very low HDL-C and lower cardiovascular risk.
Simply measuring the HDL cholesterol content, therefore, may not accurately reflect its function. While we do not have easily available tests to measure HDL function, we can potentially use HDL particle assessment as well as the company it keeps (i.e. low triglycerides, larger less dense LDL particles) to better assess the potential benefits of HDL. Thus, if there is any concern about potentially dysfunctional HDL, I usually recommend advanced lipid testing to see the specific subtypes of HDL.
What can we conclude from all the HDL confusion?
Raising HDL with drugs does not reduce cardiovascular events, yet having a naturally low HDL is associated with increased risk.
The best answer, therefore, is to live a lifestyle that helps you have a “not low” HDL level. This means first and foremost avoiding the medical conditions associated with low HDL (i.e. insulin resistance, diabetes, and metabolic syndrome).
Textbooks predictably state the interventions to naturally raise HDL include exercise and moderate alcohol intake. Unfortunately, these have minimal effects. In fact, they pale in comparison to a low carb high fat lifestyle. In my 20+ years in the medical field, I have never seen an intervention as effective as LCHF in raising HDL, and the studies agree.
This brings us back to our question once again.
Why are HDL levels important?
HDL levels are important because it is a reflection of our underlying metabolic health and our lifestyle. A properly constructed LCHF lifestyle lowers triglycerides, raises HDL, and reduces the small dense LDL, among other benefits. Such a lifestyle likely reduces overall cardiovascular risk and will likely be shown to improve longevity and health span. While HDL may not be the main reason for this, we can’t ignore its role simply because it is more nuanced than “good” and “bad” cholesterol.
My advice, therefore, is to see the whole picture. Embrace the nuance. And make sure you get a thorough and proper evaluation of your cardiovascular risk.
If you are hungry for more, I created my Truth About Lipids program, a program focused on Cholesterol, to help break through the confusion and provide you with everything you need to thoroughly understand cholesterol and its impact on your health.
Learn more: Truth About Lipids Program
If you still have questions, you may want to consider a one-on-one health coaching consultation so you can get the individual attention you deserve with a thorough assessment of your lifestyle and its impact on you as an individual.
Please comment below if you have any questions or comments that may help further the discussion.
Thanks for reading.
Bret Scher MD FACC
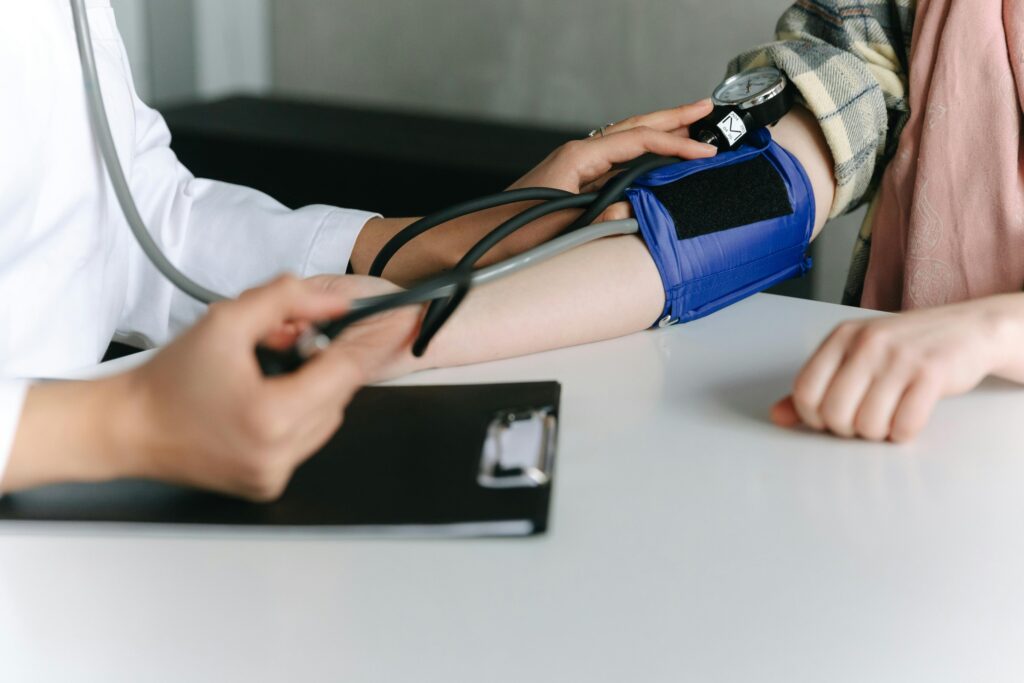
Did you know changing the way you eat may be able to normalize your blood pressure completely? For many people it’s true. But what’s surprising is that it isn’t changing to the diet that most doctors and dieticians recommend.
The DASH diet, Dietary Approach to Stop Hypertension, has long been the “go-to” diet for reducing blood pressure. The DASH diet is a high carbohydrate, low fat diet that recommendseating plenty of fruits, veggies, whole grains, and limiting salt and saturated fat. And while that works for some people, many others can normalize their blood pressure with a nearly opposite approach.
A 2023 study published in The Annals of Family Medicine, demonstrated that a very low carbohydrate diet with no limitations on the amount of salt or the amount or type of fat eaten was better at lowering blood pressure compared to the DASH diet.
Many wonder how this could be, but the answer is pretty straightforward.
Poor metabolic health, from insulin resistance to type 2 diabetes, is a leading cause of high blood pressure. And low carb diets are one of the best lifestyle approaches for improving or even normalizing metabolic health. Therefore, it makes complete sense that a low carb diet would be highly effective at normalizing blood pressure.
Of course there are many other ways to improve blood pressure, such as quitting drugs, tobacco and alcohol, getting regular exercise, managing stress, etc. And these are very important. But since everyone has to eat, it is powerful to eat in a way that can normalize blood pressure.
Let’s explore four ways how low carb diets can help blood pressure.
1- Weight loss
Having overweight or obesity is a strong contributing factor to high blood pressure. And while low-carb eating isn’t the only way to lose weight, it tends to be as good as or even better than low fat eating for weight loss. Some publications even demonstrate weight loss on par with highly effective GLP1 weight loss drugs like Ozemipic and Wegovy.
2- improved metabolic health
As mentioned, metabolic dysfunction is a clear trigger for elevated blood pressure. And while low carb eating isn’t the only way to improve metabolic health, it is likely the most effective dietary pattern for improving metabolic health, and can even do so with or without weight loss.
3- Ketosis
If someone lowers their carbohydrate intake enough, they can enter a state of ketosis, a normal physiologic state where we burn primarily fat for energy instead of carbohydrates. When this occurs, our insulin levels drop to a normal level and we have a natural diuresis, meaning we eliminate sodium and water more than usual. This can help lower blood pressure above and beyond weight loss.
4- Avoiding processed foods
Most well formulated low carb diets avoid highly processed junk foods like potato chips, candy, doughnuts, etc. that can lead to high blood pressure. So, simply eliminating these foods can also contribute to lower blood pressure.
What about salt?
One of the big misconceptions about blood pressure is that we all need to lower our salt intake for better blood pressure. However, this appears to be a gross over-generalization. There’s a growing understanding that a minority of individuals have “salt sensitive” hypertension. This means that the majority are unlikely to affect their blood pressure by altering their salt intake.
Furthermore, where we get our salt likely makes a difference. For insurance, if someone is getting their salt from highly processed foods like chips, pretzels, etc, they are hit with an ultra-processed combination of salt, calories, carbs, and sugars that is bound to raise blood pressure.
But what if someone is eating whole foods like broccoli, cauliflower, steak, and avocado, and they add salt to that meal? Clinical experience suggests our bodies react much differently to this type of salt exposure, and people can dramatically lower their blood pressure despite adding salt to their diet.
Low Carb Eating Works
So while it may not be the right approach for everyone, it is increasingly clear that eating a well-formulated low carb diet is a safe and effective way to lower blood pressure. It’s time to include low carb diets as a first line treatment option for normalizing blood pressure.
Thanks for reading!
Bret Scher MD FACC

Is the Keto Diet Heart Healthy? 7 Reasons Why This Cardiologist Agrees
I am a board certified, card-carrying cardiologist, and I want my clients to eat more fat, more meat, more cheese, more eggs, more avocado, more, more, more.
For decades medical establishments have convinced us to eat low fat, higher carb diets. How has that worked for our health? Here’s a hint, we have record numbers of obesity, diabetes and dementia. Yet, as a cardiologist, that’s the party line I am supposed to support.
But I can’t. It’s just wrong, and I can’t support that line of thinking, not for a second.
Instead, I am a Low Carb Cardiologist. Here are the top Seven reasons why
- Reducing Insulin is Essential to Health and Weight Loss.
Insulin is a hormone naturally secreted by the pancreas to help regulate blood sugar levels. Everything we eat (except possibly for 100% fat meals) causes insulin to rise. That is normal physiology. The problem occurs when our bodies become resistant to the effects of insulin, thus requiring our pancreas to make more and more and more insulin.The problem? Insulin promotes fat storage, increase inflammation and oxidation, and can even help fuel the growth of cancer cells. Therefore, the healthiest approach is one which reduced the level of insulin to the lowest possible levels. As it happens, a Low-carb High-fat or ketogenic lifestyle (LCHF/Keto lifestyle) dramatically improves your body’s sensitivity to insulin, reduces the amount of insulin secreted, and it allows your body to naturally use your fat stores for what they are designed for: Break them down into energy! Once we see that we need to fight chronic elevations of insulin, it becomes obvious why a low-fat diet is harmful, and why a low carb diet is the true path to health. - Eating Fat Improves Your Cholesterol!
Wait, what? Eating fat can improve my cholesterol? Sounds crazy, right? That goes against everything we have heard from the medical establishment. Notice I said “cholesterol.” I didn’t say the “bad” low density lipoprotein (LDL), I didn’t say the “good” high density lipoprotein (HDL), or any one specific type of cholesterol. We have over emphasized the solitary variable of LDL for too long. Total cholesterol to HDL ratio, Triglyceride to HDL ratio, lipoprotein size and density, insulin sensitivity, and other metabolic measures are more powerful predictors of cardiovascular health than just LDL.Once again, we see that all these markers improve with a Low Carb High Fat (LCHF) lifestyle. The medical establishment needs to realize that we are more complicated than one lab value. The key is to look at the whole picture, and this picture dramatically improves with a LCHF lifestyle.If you want to learn more about lipids and cholesterol, I recommend checking out my new dedicated cholesterol course: The Truth About Lipids. - Higher HDL is Associated with a Lower Risk of Heart Disease.
HDL is your friend, but drugs are not. Observational evidence has consistently shown that higher HDL is associated with a lower risk of cardiovascular disease. However, our healthcare establishment does not prioritize HDL for one simple reason- Drugs that raise HDL don’t make you healthier. Trial after trial has failed to show any benefit from drugs that significantly increase HDL.Instead, it’s the HDL-raising lifestyle that provides the benefit, not artificially increasing it with drugs. What’s the best lifestyle to naturally raise HDL? You guessed it. LCHF/Keto lifestyle. Add in some resistance training and you have your friendly HDL climbing the way it was meant to…Naturally. - LCHF Leaves You Feeling Great, Leading to Healthier Decisions
What kind of health decisions do you make when you are fatigued, achy, and find it difficult to concentrate? That’s a rhetorical question, I already know the answer. When things look glum and we don’t feel well, it’s far too easy to sit on the couch or reach for the chips and cookies. Compare those decisions to those you make when you are well rested, energetic, and seeing the world more clearly. For most people, the better you feel, the better decisions you make.Guess what? The majority of people who change to a LCHF lifestyle feel better! It may take a few days or weeks, but in general, they feel more in control of their health, more energetic, and they are able to make better health decisions. I admit this is difficult to prove in a scientific trial. That is why we all should become our own n=1 scientific trial. How do you feel and how are your health decisions after going to a LCHF lifestyle? What matters most is what works for you, not what works for hundreds of people who are kinda-sorta like you. - Keto helps you with fasting.
Eating better helps you not eat. People who eat a high carb diet eat a lot, don’t they? They are always grazing and snacking. Our bodies go through the roller coaster of blood sugar and insulin spikes, making it a challenge to go 24, 18, or even 6 hours without eating. This creates a constant, unwavering supply of insulin in our blood stream.Why is this harmful? For one, it promotes fat storage and keeps us from using our fat as fuel. Secondly, chronically elevated insulin can predispose to heart disease, strokes, cancer, dementia and other devastating health conditions. When people change to Keto, however, they realize they do not need to eat nearly as much or as frequently. Avoiding the carbs and increasing the fats keeps us full longer, and our bodies quickly adapt to longer periods without eating. The result? We can use our fat stores for what they were designed- a source of fuel! It also allows our body to maintain lower insulin levels, and also allows our cells to take care of their health chores, referred to as Autophagy.If you’re interested in Fasting and want to make sure you’re doing it correctly, download my free Full Guide to Fasting. - LCHF Promotes Health Through Increased Autophagy.
Autopha-What? In medicine we like using fancy words to make us look smart. Autophagy is a big word to describe cellular housekeeping. When we have low enough intake of carbs and protein, or when we do intermittent fasts, our bodies can take care of their “to do” lists. That list includes breaking down weak or damaged cells, recycling the good parts and discarding the rest, and slowing down the processes that can lead to abnormal cell growth (i.e. excess proteins in Alzheimer’s disease, abnormal cancer cells etc.).Admittedly, long term outcome studies evaluating fasting or LCHF and cancer or dementia risk have not been done. But, on the flip side, drug trials to prevent the same are showing no benefit despite hundreds of millions of dollars invested. If you asked me (which you sort of did since you are reading my article), I’d vote for autophagy as a preventative strategy any day. It makes good physiologic sense, and it is so easy to achieve. - With Keto You Will Enjoy Eating Again!
That’s right. A way of eating that helps you lose weight, helps you feel better, improves your health and is actually enjoyable! No fake processed soy products, no cardboard tasting rice cakes. True, it also means no more candy, processed snack foods, doughnuts and danishes. But once you swear them off for a few weeks, and you are eating all the eggs, avocados, nuts, fish, steak, cheese etc. that you want, you won’t miss those old crutches any more. Let the enjoyment begin!
I could go on, but since it seems people like “7 Reason” articles, I will leave it at that.
Now you know the secret: Look at the whole picture. Look for a lifestyle, (not a diet) that helps you feel better, increases your enjoyment, and still benefits your overall health.
Is LCHF/Keto the right lifestyle for you? It just may be. To learn more about Low Carb and Keto, download this free E-Book:
Thanks for reading,
Bret Scher, MD FACC
Founder, Boundless Health
www.LowCarbCardiologist.com
ADDENDUM!!
Since I have published this article, there has been a windfall of media buzz around low carb diets increasing our risk of heart disease or diabetes. Let’s look at where that information came from.
1- A study force feeding mice excessive amounts of industrial omega 6 oils. You can guess what I have to say about that. The article was incredibly helpful, and I immediately stopped force feeding my pet mice industrial seed oils. Thanks goodness for that article. As for how it applies to humans eating real food that contain fat, there is zero correlation.
2- Epidemiological study suggesting those who ate low carb (40% calories from carbs, which by the way is NOT low carb) as measured by two food journals over 25 years had a higher risk of dying. Oh and by the way, at baseline they were heavier, more sedentary, smoked more, and ate fewer veggies. Yet somehow they concluded it must be the low carb diet that “caused” the harm. Once again, it may not be bad science, but it sure was awful interpretation of the science.
In light of those two studies and the hoopla surrounding them, has anything happened to change my mind about a LCHF/keto diet being beneficial for our overall health and our heart health?
Absolutely not.
We still need to individualize our care and our lifestyle for who we are and how our bodies respond. That is always the case regardless of our nutrition, our medications, our exercise etc. As long as we do that, then this cardiologist still believes that LCHF IS HEART HEALTHY!
If you liked this post, you’ll love my free E-Book on Low Carb/Keto Starter tips to help you get started on your LCHF path!
Thanks for reading.
TAKING YOUR NEXT STEP
WITH BOUNDLESS HEALTH AND DR. SCHER
We are excited to help you in your quest for better health! If you are ready to take the next step, your annual membership will give you access to:
START A CONVERSATION
Connect with Dr. Scher to see if this model is right for you today.
Let’s Talk
Send us a message and let us know how we can help you.
